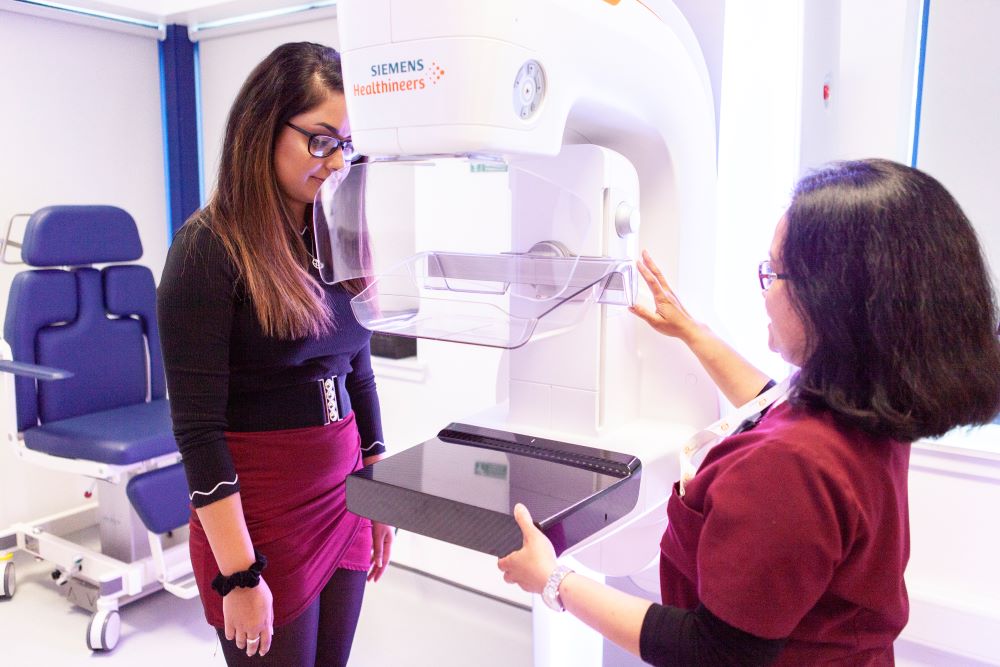
What is mammography?
Mammography has been around for decades and is generally used for three reasons:
- Screening – This is for people at average risk of breast cancer who undergo routine mammography to find cancers that are not yet symptomatic.
- Surveillance – This refers to women that are at a high risk of breast cancer and who undergo frequent mammograms.
- Diagnostic – When a woman has symptoms (such as a lump in the breast) and has a mammogram to help in diagnosing what the problem is.
Generally speaking, when it comes to screening, the mammogram routinely used is the 2D mammogram. Put simply this comprises of 2 imaging plates, with the breast between them, and an X-ray image is taken across the breast.
The 3D mammogram
The 3D mammogram (also known as tomosynthesis) is carried out much in the same way as a 2D mammogram however it can image multiple layers of the breast, thus giving a 3D image as opposed to a 2D one.
This reduces overlapping tissue, which is a common reason women are brought back for extra pictures after a standard screening mammogram.
The benefits
- Reduces the need of follow up imaging
Occasionally a 2D mammogram will show up a potential abnormality that needs further evaluation using 3D mammography. Having a 3D mammogram from the start can reduce this added test and anxiety caused by having to wait for it.
- Detects slightly more cancers than 2D mammography alone
1 more breast cancer can be found per 1,000 women screened using 3D mammography vs 2D alone.
- Improves breast cancer detection in women with dense breasts
Dense breasts make interpreting a 2D mammogram challenging. This is made easier using 3D imaging.
Of note is that an increased breast density in 75% or more of the breast is associated with an almost 5-fold increased risk of developing breast cancer, and this risk continues over an extended period of time.
Any negatives?
When it comes to comparing 3D vs 2D imaging it would seem only logical that 3D screening is the better option and surely life-saving if it showed up a small symptom-less cancer, but yet to date there is still no definitive evidence that 3D scans save more lives than 2D. There are studies currently ongoing looking into this topic (TIMST study)1.
The breast screening debate
Breast screening as a whole has caused much controversy over the years. This is because the evidence to date doesn’t conclusively show that lives are saved through screening for breast cancer. Surprised to hear this? You’re not alone.
In fact, not only has screening not shown to reduce the death rate from breast cancer, but it has also been known to lead to false positives and over-diagnosis. This alone causes a lot of stress and anxiety, plus further invasive testing and sometimes even inappropriate treatment.
Of course it is important to emphasize the use of the term ‘screening’ here. This refers to women with no symptoms (no lump/no breast changes or concerns) and no history that puts them at higher risk of breast cancer (i.e. BRCA gene).
However, breast screening is a population screening method as well as an individual screening one. For the woman who wishes to be in charge of her health, wishes to be proactive and accepts the pros and cons of screening procedures, should mammography screening not be a choice rather that a dictated public health matter for populations as a whole?
Going forward
When it comes to screening and breast concerns, the best advice is always to see a healthcare specialist and consider your imaging options.
At ROC we are delighted to be able to offer our patients the opportunity to benefit from our One-Stop Clinic service. This provides a triple assessment of any breast abnormalities including consultation and examination with one of our experienced breast surgeons, mammography or ultrasound examination, and fine needle biopsy if required. This produces a full diagnostic assessment in one appointment and reduces the time between initial investigation and diagnosis, helping to reduce anxiety for patients.
Breast health is also an important part of our Well Woman health checks, which have packages that include breast examination and mammography.
To find out more or to book an appointment, fill in the form, call us on 01224 515 254 or email aberdeen@rochealthservices.com
1, https://ecog-acrin.org/tmist


